Before the COVID-19 pandemic, tuberculosis (TB) was the leading cause of death from a single infectious agent in Indonesia—making TB one of the country’s top priority health focus areas, with the aim to reduce the disease incidence from 354 (in 2021) to 65 per 100,000 people by 2030.
To combat it, Indonesia’s Ministry of Health (MOH) invested in the development and implementation of a national TB information system (SITB) that collects case management and logistics data at the facility level. SITB has emerged as Indonesia’s latest platform for reporting TB cases since 2020. It has been adopted by health care providers nationwide, including primary care facilities, hospitals, districts, provincial health offices, and the MOH.

However, the system is not interoperable with other facility-based information systems, leading health workers to enter the same or similar TB data in duplicate into multiple different systems. This means that health workers are spending valuable time entering data into systems, and not focusing on provision of quality health services. To address this issue, CHISU is supporting Indonesia’s MOH in the roll out of the national health information exchange platform—SATUSEHAT—to improve the exchange of TB and other health data within and between health facilities and program-specific systems like SITB.
To improve the exchange of TB data, the MOH and CHISU developed a generic interoperability platform using the digital health global good Open Health Information Mediator (OpenHIM). This platform will allow data to flow between primary health care facilities’ information systems and SITB using SATUSEHAT. The use of OpenHIM serves as an additional pathway for health facilities, district and provincial health offices, and various health programs to exchange data with SATUSEHAT, since some entities might have difficulty adapting their systems to be compliant with Fast Healthcare Interoperability Resources (FHIR)—a standard that defines how different systems exchange health care information despite how it is stored in them. The generic interoperability platform will provide this data exchange service for facilities, offices, and programs experiencing such difficulties.
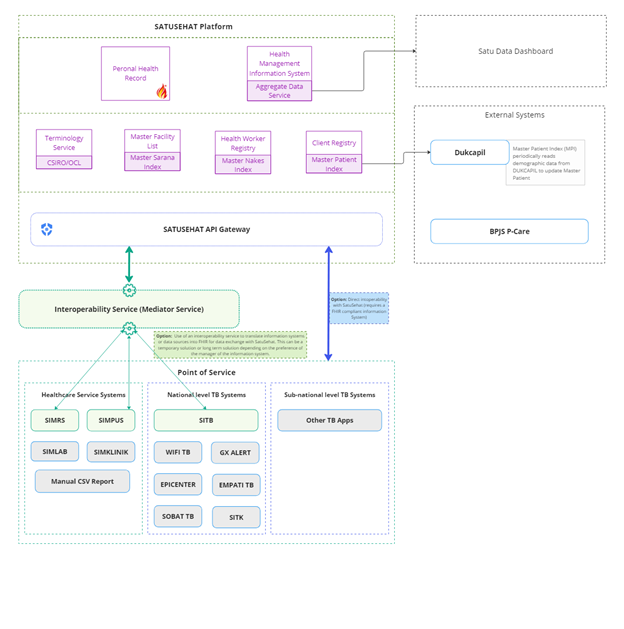
In practice, the improved interoperability will allow facility staff to capture data just once (instead of capturing duplicative data) in their facilities’ information systems—and this data will automatically be pushed to SITB via SATUSEHAT for reporting and case management purposes.
One of Indonesia’s major vendors of primary care facilities’ information systems recently conducted a thorough testing of the CHISU-supported generic interoperability platform and its connection to SATUSEHAT. The findings were highly promising, as the platform enabled a seamless flow of data between facilities and SITB. This accomplishment serves as a testament to the platform's efficacy in promoting interoperability and efficient data exchange. Also, CHISU has conducted interoperability assessments that aim to oversee the current condition and capability of health information systems, and to see what the potential is for expanding the generic interoperability platform at the subnational level. The goal is to ensure seamless management of TB cases data from all facilities, allowing for streamlined and efficient processes.
“We thank CHISU for providing this technical assistance for the Sidoarjo district to accelerate the interoperability and connection to SATUSEHAT,” said the Head of the District Health Office Dr. Fenny Apridawati, S.KM, M.Kes. “Interoperability of health systems has indeed become a focus for the district and has received full support from the local government; it is also a focus of the Head of District (Bupati), who has been very supportive of this activity.”
Overall, it’s expected that by improving the exchange of TB data, interoperability between SITB and primary care facilities’ information systems will remove duplicative data capture by health facility staff, improve data availability, and support timely decision making. By increasing the availability of interoperability pathways, this will also reduce the risk of data omission and reduce data entry burden, improving case and treatment management—which will ultimately enhance health outcomes and move the needle toward achieving Indonesia’s TB elimination goals.